
In the current issue of Vision Development & Rehabilitation, Bob Sanet, Pilar Vergara and I have a Perspective piece in which we review a Paradigm Shift in the Treatment of Amblyopia. The article resurrects a formula proposed by Dr. Arnold Sherman to provide a more accurate measure of the extent of treatment success in amblyopia, now that current research has squarely positioned the condition as a binocular problem in which visual acuity is simply one monocular sign. Sherman notes that Mayer and colleagues proposed an Amblyopia Success Index (ASI) based on visual acuity as follows:
ASI = (Initial VA – Final VA) / (Initial VA – Test Distance) x 100. As an example, if the initial acuity was 20/60 and improved to 20/30, the ASI = (60- 30/60-20) = (30/40) x 100 = 75%.
Given the significance of amblyopia as a binocular problem, Sherman proposed an analogous Binocular Success Index (BSI) using Wirt Circle Stereopsis (WS) in seconds of arc as a guide. A maximum value in most commercially available tests of 20 seconds of arc is the constant. His formula is: BSI = (Initial WS – Final WS) / (Initial WS – Maximum WS) / x 100.
As an example, if initial stereo acuity was 100 seconds of arc and improved to 30 seconds of arc, the BSI = (100-30) / (100-20) = (70/80) x 100 = 88%. He suggested that the more appropriate index of success in amblyopia would be the average of the ASI and BSI, in this instance (75 + 88) / 2 x 100 = 82%.
While the numbers in Sherman’s example don’t seem significant when differentiating between a 75% level of success and an 82% level of success, combining ASI and BSI obviously becomes more significant when stereopsis improves to a considerably greater extent that visual acuity. For example, using the formula for ASI, a patient who improves from 20/50 to 20/40 would be assigned a success index of only 33%. But if that patient improved from 100 seconds of arc to 20 seconds of arc, BSI is 100% which doubles the overall success index to 67%.
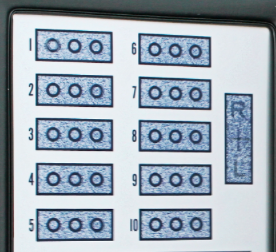
For many years we have routinely conducted the Wirt Circle test on all of our patients (with or without amblyopia). In all of our patient reports I have included this phrase: “Stereopsis is a sensitive index of binocular function. On the Wirt Circle Test, ________ scored at the level of X% accuracy.” In other words, if 5 out of 10 are correct, the patient is assigned a score of a 50% level of accuracy. While I realize this isn’t as sophisticated or technically as accurate as Dr. Sherman’s index, it is a justifiable simplification of the test result. That way, when we re-test with a suitable lens/prism Rx, or after vision therapy, we can say that the patient improved from X% level of accuracy to Y% level of accuracy.
Nearly 30 years ago, in an article in the Journal of Behavioral Optometry, Dr. Selwyn Super pointed out some of the nuances of stereopsis testing. He made the observation that speed of the stereopsis response may prove to be just as valuable as the stereo acuity measure in seconds of arc. When taking visual acuity measures, the patient with amblyopia takes longer to respond, particularly as we approach the limit of their visual resolution, so this lag in the speed of stereo acuity responses is not entirely surprising. Although he introduced a test for the speed of stereopsis based on Wirt Circle responses that was distributed by OEPF, it was ahead of its time and removed from the market. There is reference to this test in a master’s thesis on file with Pacific U. College of Optometry. It remains a valuable concept, and would be another potentially useful metric in differentiating amblyopia and documenting response to treatment.

I just did a quick survey of ODs on Facebook, a community of primary care optometrists, posing this question: Does your office routinely test stereopsis on all pediatric patients? Please indicate “yes” or “no”. Realizing that this isn’t a scientific survey since it wasn’t “anonymous”, and the people who don’t do the test tend not to answer in a forum of that nature, it was still encouraging to note that among the first 200 respondents there were 197 yes and 3 no. Although I didn’t ask respondents to indicate how many considered themselves primary care optometrists, it would be reasonable to expect that the high majority are. A public word of thanks to all those who responded.
If our premise regarding amblyopia is correct, that stereo acuity is a sensitive index of binocular function, most primary care optometrists have a tool at their disposal that they’re already using that will help facilitate the paradigm shift in amblyopia from a monocular emphasis to a binocular balance.
Excellent article Bob and Pilar and excellent reporting Len
Thanks, Bubba!